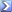Weird race based morbidity stats
#1
From the CDC website: https://www.cdc.gov/coronavirus/2019...iew/index.html
With an ‘n’ as big as this group you’d expect even a 1.3 relative risk to have a p value of less than 0.05...

With an ‘n’ as big as this group you’d expect even a 1.3 relative risk to have a p value of less than 0.05...

#2
Not adjusted for comorbidities, or socio-economic conditions. So no real surprise if you consider those factors.
Hard to draw any conclusions about innate ethnic biological susceptibility without adjusting for health, living conditions, cultural behavior patterns, etc.
Hard to draw any conclusions about innate ethnic biological susceptibility without adjusting for health, living conditions, cultural behavior patterns, etc.
#3
Not adjusted for comorbidities, or socio-economic conditions. So no real surprise if you consider those factors.
Hard to draw any conclusions about innate ethnic biological susceptibility without adjusting for health, living conditions, cultural behavior patterns, etc.
Hard to draw any conclusions about innate ethnic biological susceptibility without adjusting for health, living conditions, cultural behavior patterns, etc.
#4
Gets Weekends Off
Joined APC: Jul 2011
Position: Under beer over couch after skool
Posts: 316
From day one in dealing with this “people have been saying” ACE2 gene expression is likely linked to negative outcomes like it was in SARS and other Corona viruses. Whether ACE2 expression increases with age and is different between races and genders is an important question.
Now that racial disparity is available it would be interesting to look at several avenues to understand COVID outcomes.
I’d say practical economic factors like health insurance, availability of sick leave, ability to take a pay cut or miss work, and distrust of medical treatment are probably heavily involved in the disparity. I’d also posit that lower income neighborhoods are frequently located near industrial centers, where air pollution could influence ACE2 expression.
Here’s one review on it. I’ve seen some articles on the racial disparity in the NYT, Atlantic and or Ars Technica.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7499935/
Now that racial disparity is available it would be interesting to look at several avenues to understand COVID outcomes.
I’d say practical economic factors like health insurance, availability of sick leave, ability to take a pay cut or miss work, and distrust of medical treatment are probably heavily involved in the disparity. I’d also posit that lower income neighborhoods are frequently located near industrial centers, where air pollution could influence ACE2 expression.
Here’s one review on it. I’ve seen some articles on the racial disparity in the NYT, Atlantic and or Ars Technica.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7499935/
#5
It could also be just locale. Big cities with high population densities have historically been the worst place to be in a pandemic. Just too dang many chances to get it. Nonetheless, a four-fold difference in hospitalization rates with an ‘n’ this big is a HUGE difference.
Thread
Thread Starter
Forum
Replies
Last Post